For years, the general public: and many insurance adjusters: have viewed orthodontics as a "luxury" or purely cosmetic service. We know the truth: a straight smile is often the byproduct of a healthy, functional bite. But as any orthodontist will tell you, the gap between knowing a treatment is necessary and getting an insurance company to pay for it can feel like a canyon.
Navigating the world of "medical necessity" is one of the most significant challenges in modern orthodontic practice. If you don't cross every 't' and dot every 'i' in your documentation, your claims will be relegated to the "cosmetic" pile, leaving your patients with higher out-of-pocket costs and your practice with administrative headaches.
At ALS Billing, we specialize in helping providers bridge this gap. Whether you are transitioning into more complex cases or simply want to ensure your revenue cycle is optimized, mastering the art of proving medical necessity is your first step toward success.
What Exactly Is "Medical Necessity" in Orthodontics?
In the eyes of most payers, medical necessity is determined by the presence of a "handicapping malocclusion." This isn't just a fancy way of saying "crooked teeth." It refers to conditions that significantly impact a patient’s physical health, oral function, or overall quality of life.
Because criteria can vary wildly between private payers and state-funded programs like Medicaid, your documentation must be ironclad. You aren't just a clinician; in the billing world, you are a storyteller who must prove why this specific patient needs this intervention to thrive.

The "Golden Tickets": Automatically Qualifying Conditions
There are certain scenarios where the burden of proof is significantly lower because the condition is universally recognized as medically necessary. These are your "strongest" cases for approval:
- Cleft Palate and Craniofacial Anomalies: Conditions like Cleft Lip, Cleft Palate, Crouzon Syndrome, or Hemifacial Hypertrophy almost always qualify. These involve systemic or congenital deformities that require reparative orthodontic work.
- Traumatic Injury: If a patient has suffered a significant orofacial injury that requires orthodontic intervention to restore function, insurance is much more likely to step in.
- Severe Functional Impairment: This includes documented respiration or speech pathologies that are directly exacerbated by the patient’s malocclusion.
- Psychosocial Impact: In some cases, mental, emotional, or behavioral problems (such as severe social withdrawal or low self-esteem documented by a mental health professional) linked to the malocclusion can meet the criteria.
For more on how specialized billing can help these complex cases, check out our guide on why your revenue cycle might be underperforming.
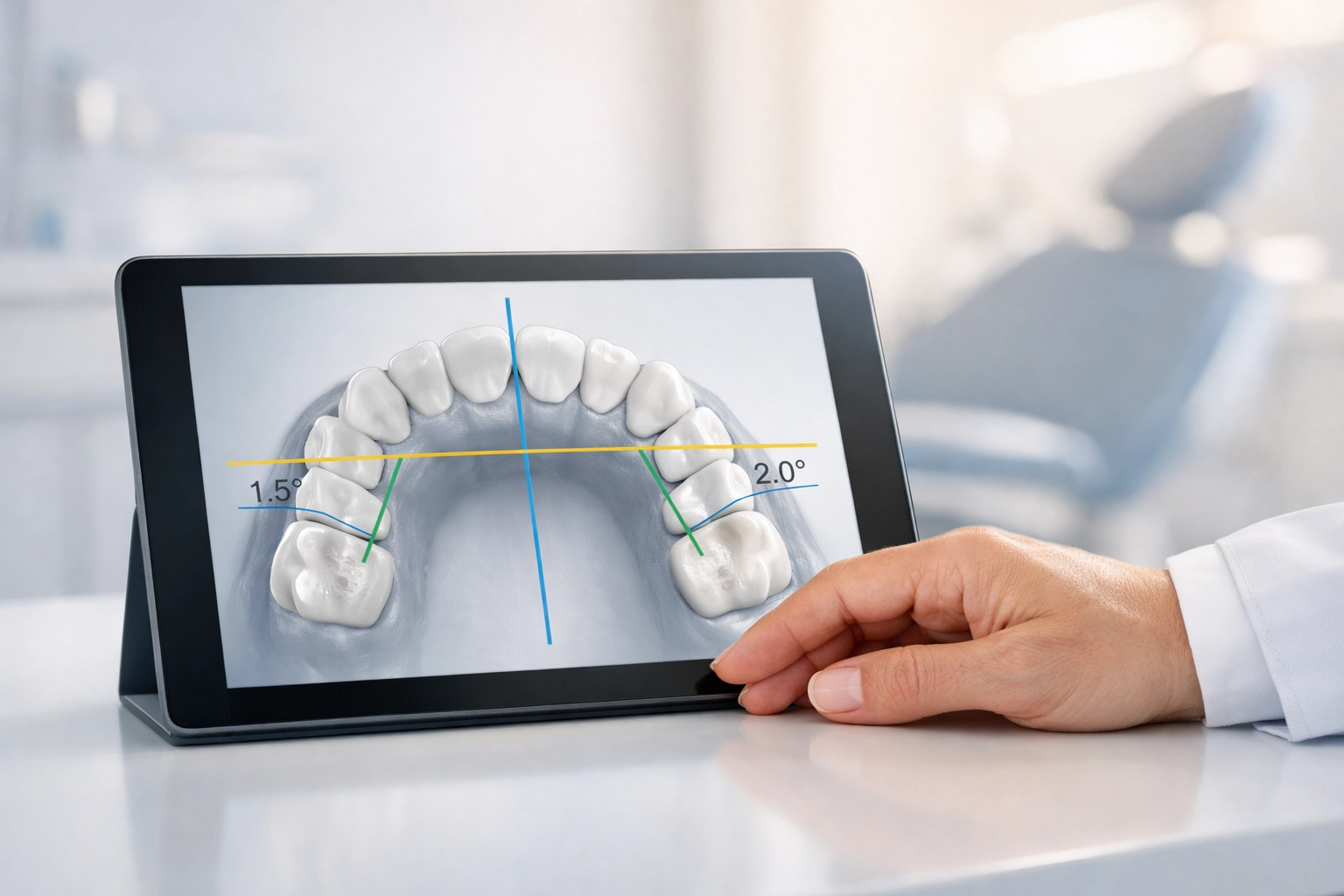
The Numbers Game: Measurable Occlusal Criteria
When a patient doesn’t have an automatically qualifying condition, you have to lean on the numbers. Insurance companies love data. To secure approval for "medically necessary" treatment, you typically need to document measurements that hit specific thresholds:
- Overjet: 9 mm or greater.
- Reverse Overjet: 3.5 mm or greater.
- Crossbite: Anterior or posterior crossbite affecting three or more teeth per arch.
- Open Bite: Lateral or anterior open bite of 2 mm or more affecting four or more teeth per arch.
- Crowding/Spacing: 10 mm or more in either the maxillary or mandibular arch.
- Impinging Overbite: When the teeth are making contact with soft tissue, causing documented trauma or recession.
Using standardized tools: like the HLD (Handicapping Labio-Lingual Deviation) index: is essential. If you aren't already using these scoresheets, you are likely leaving money on the table and inviting denials.
The Paperwork Trail: Documentation Requirements
If you didn’t write it down, it didn’t happen. This is the mantra of medical billing. To master medical necessity, your clinical records must be comprehensive and include:
- The Clinical Assessment: A detailed narrative from the orthodontist explaining the functional deficits.
- Diagnostic Material: Digital study models (which are increasingly preferred over physical casts in 2026), full-mouth or panoramic X-rays, and cephalometric films.
- Physician Collaboration: This is where many practices stumble. If you are claiming medical necessity due to a speech impediment or a respiratory issue, you need a letter from a licensed physician, speech therapist, or respiratory therapist. Their professional opinion carries immense weight in the pre-authorization process.
- Patient Compliance: Documentation that the patient is a good candidate for treatment, meaning they have addressed active dental diseases like caries or periodontitis first.
Are you worried your current documentation might be a red flag? You might find our post on why late notes and out-of-order billing are audit magnets particularly helpful.
What Does NOT Qualify?
Knowing what to avoid is just as important as knowing what to include. Spending hours on a pre-authorization for a case that will never be approved is a drain on your staff’s time. Generally, the following do not meet the "medical necessity" bar:
- Minor to moderate Class II or Class III malocclusions without functional impairment.
- TMJ clicking or popping without other symptoms or documented pathology.
- Thumb-sucking habits (unless they have led to one of the measurable criteria mentioned above).
- "Phase II" treatment if the "Phase I" treatment already resolved the qualifying medical condition.
Why USA-Based Security is Non-Negotiable
In the orthodontic world, you are dealing with sensitive patient data, including X-rays, photos, and personal medical histories. As we move further into 2026, the risks associated with data breaches are higher than ever.
Many billing companies outsource their labor overseas to cut costs, but this often comes at the expense of security and communication. At ALS Billing, we pride ourselves on being a USA-based company. This means:
- HIPAA Excellence: Our security protocols are strictly aligned with US federal laws.
- Clear Communication: When you have a question about a complex medical necessity claim, you can pick up the phone and talk to someone who understands the nuances of the American insurance landscape.
- Speed and Accuracy: We understand the specific regional requirements for Medicaid and private payers across the country.
Outsourcing your billing isn't just about saving time; it's about protecting your practice's reputation. If you're on the fence, read our honest take on whether you really need a medical billing company.
Best Practices for Orthodontic Approval
To ensure your practice remains profitable while providing the best care possible, follow these three best practices:
1. Pre-Authorize Everything
Never start treatment on a "medically necessary" case until the pre-authorization is in hand. Retroactive approvals are incredibly rare in orthodontics and usually end in a headache for both you and the patient.
2. Educate Your Staff
Your front-desk and clinical assistants should know the basic criteria for medical necessity. If they can identify a potential "qualifying" case during the initial consult, they can ensure the correct photos and measurements are taken immediately, saving a follow-up appointment.
3. Partner with Experts
Orthodontic billing is specialized. It’s not the same as general dentistry, and it’s certainly not the same as standard medical billing. Partnering with a company like ALS Billing allows you to focus on your patients while we handle the "medical necessity" battle with the insurance companies.
We’ve seen every trick in the book from payers, and we know how to counter them with clinical evidence and persistent follow-up. You might want to see our 7 mistakes you're making with medical billing to see if any of these are slowing down your current approvals.
The ALS Billing Difference
At the end of the day, your goal is to transform lives through better oral health. Our goal is to make sure you get paid for that expertise. Mastering medical necessity is a full-time job, and in a busy orthodontic practice, you likely don't have the "free" time to manage it effectively.
By leveraging a USA-based team that understands the intersection of clinical orthodontics and insurance requirements, you can reduce your denial rate and increase your practice's bottom line.
Ready to streamline your orthodontic billing? Explore our knowledge center for more tips, or contact us today to see how we can help you master medical necessity once and for all.
